SARS survivors continued to improve at 18 years compared to 12 years after discharge. Emotional and mental health restored to the normal. However, SARS survivors still had lower quality of life 18 years after discharge than controls, mainly in physiological functioning, physical role, bodily pain, general health, vitality, and social functioning. Residual lung lesions mainly involved the upper lobe of the right lung and the lower lobe of the left lung. In addition, the lesions were mainly central-lobular nodules. Survivors of SARS and MERS also showed fibrotic abnormalities during convalescence. A follow-up study suggested that the pulmonary lesions caused by SARS-CoV infection improved mainly within 1 year after discharge but remained unchanged up to 15 years. Our study confirmed that such lesions in the lungs last up to 18 years after discharge.
Acute and postacute sequelae associated with SARS-CoV-2 reinfection (2022)
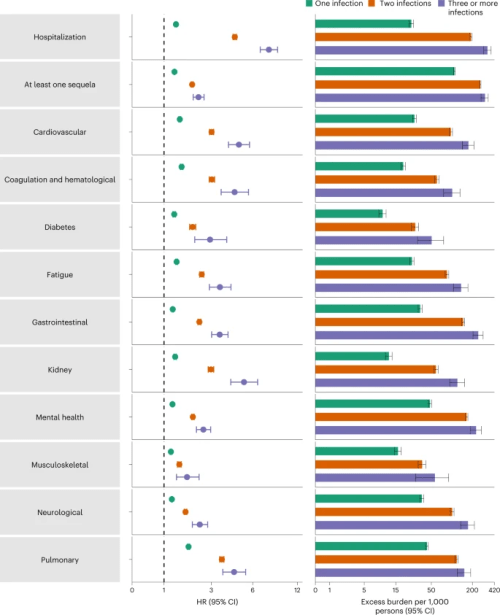
Compared to noninfected controls, cumulative risks and burdens of repeat infection increased according to the number of infections…The evidence shows that reinfection further increases risks of death, hospitalization and sequelae in multiple organ systems in the acute and postacute phase.
In sum, in this study of 5,819,264 individuals, we provide evidence that reinfection contributes to additional health risks beyond those incurred in the first infection including all-cause mortality, hospitalization and sequelae in a broad array of organ systems.

Long covid outcomes at one year after mild SARS-CoV-2 infection: nationwide cohort study (2023)
Dr. Deepti Gurdasani has a particularly good thread on Twitter about the implications of this study. The notion of “mild” COVID among young people is a false notion.


With increasing numbers infected by SARS-CoV-2, understanding long-COVID is essential to inform health and social care support. A Scottish population cohort of 33,281 laboratory-confirmed SARS-CoV-2 infections and 62,957 never-infected individuals were followed-up via 6, 12 and 18-month questionnaires and linkage to hospitalization and death records. Of the 31,486 symptomatic infections,1,856 (6%) had not recovered and 13,350 (42%) only partially. No recovery was associated with hospitalized infection, age, female sex, deprivation, respiratory disease, depression and multimorbidity. Previous symptomatic infection was associated with poorer quality of life, impairment across all daily activities and 24 persistent symptoms including breathlessness (OR 3.43, 95% CI 3.29–3.58), palpitations (OR 2.51, OR 2.36–2.66), chest pain (OR 2.09, 95% CI 1.96–2.23), and confusion (OR 2.92, 95% CI 2.78–3.07). Asymptomatic infection was not associated with adverse outcomes. Vaccination was associated with reduced risk of seven symptoms.

