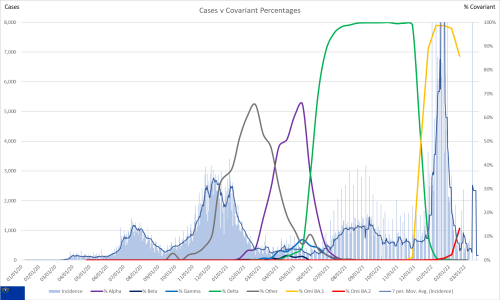
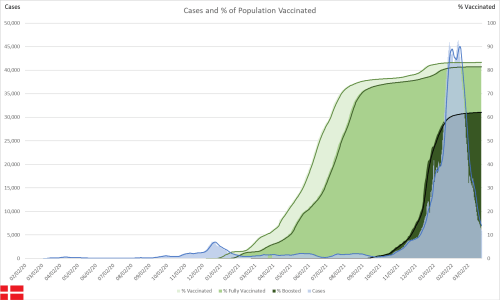
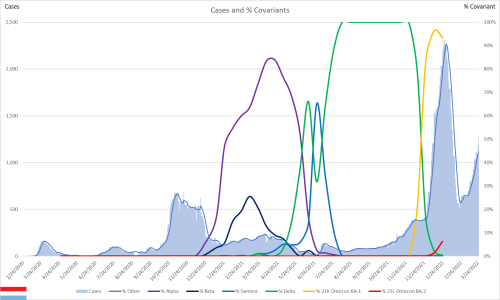
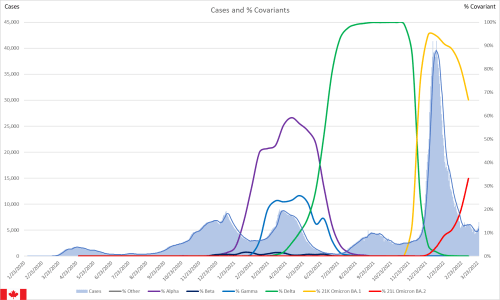
I have noticed some odd patterns in the US state data that stood out. In particular, I recall Ohio having a much higher proportion of pediatric hospitalizations than any other state. That left me wondering if other states that have reported pediatric hepatitis have had a higher proportion of pediatric hospitalizations as well, especially in comparison to states that have reported that they are not investigating any at this time. The statements for each state with hepatitis counts are taken from this website for TODAY, dated May 6, 2022.
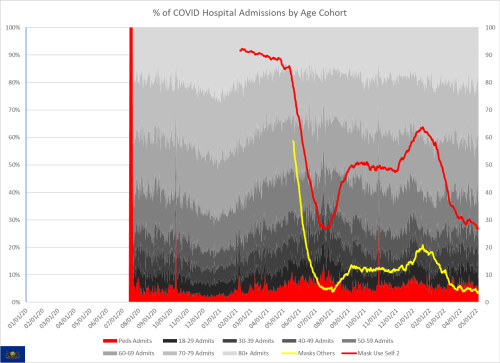
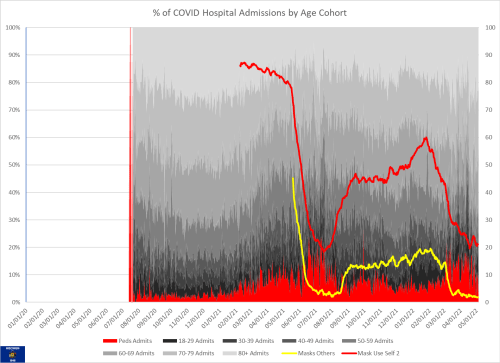
I didn’t know exactly what I would find but my hunch was correct. I’m comparing states with pediatric hepatitis to those without. This can be done with the data itself, but I wanted to see if there was any visual differences that were obvious. It is quite clear that those states with a higher percentage of pediatric hospitalizations had a larger chance of having pediatric hepatitis.
The next piece I was going to add was a stringency index to see what kind of correlation there was with hospitalizations, but then I realized that I only had that data for nations, not US states.
Given my priority is prevention, the obvious piece was to look at how the lack of masks might be a part of the problem so I recreated all of the graphs with self-reported mask use rates and estimates of the use seen by others. The mask use is reflected on the right hand scale. Normally I would label these more carefully but I really wanted to get this information out, with the hopes of maybe influencing some policy as the BA.2 surge ramps up.
One thing to note is the consistently wide difference between self-reported mask use and what the same people perceived as use by others. Self-reporting is a known common problem in survey data in that people often want to make themselves look better in the data. This phenomena is known as social desirability bias. What is important to realize is that the true estimate is likely much closer to what is reported as percentages of the use by others (the yellow line).
Recall that the omicron BA.1 surge started around the end of November, which corresponds well with the rise in the pediatric proportion of hospitalizations in most states (again, except Ohio). That lends some support to hepatitis being associated with the omicron strains, although clearly it’s impossible to prove causation and may only be a temporal association. Given that pediatric hospitalizations were higher during this period though, it would seem to suggest that COVID, particularly omicron, is playing a causal role in the disease pathway.
Just a quick aside about Ohio. I’ve been watching pediatric hospitalizations there and have a very strong suspicion of what may be behind it. It could very well be due to a surface chemist by the name of Douglas Frank. He started a Facebook group at the beginning of the pandemic called “Dr. Frank Models” where he was going on about his expertise in modeling pandemics and predicting only about 1500 deaths in the US. Anyone that tried to counter his arguments were booted from his group, so it became an echo chamber of conspiracy theories as well as anti-mask and anti-vax propaganda. The group went through a couple of name changes and eventually was removed from Facebook. He claims that Facebook took it down, but I suspect that he and his admins did so because the evidence against his claims became so damning. It had grown to over 50,000 members. He relished in the attention and was always self-promoting himself to try to get news interviews. He is adept at making things look like advanced science and mathematics, but he’s really just playing off the lack of education among many of his followers who wanted something good to believe about the pandemic.
I also suspect that since he was doing all of this self promotion and getting on local media in Ohio as well as being asked to speak on the pandemic, many people in the state got on board with his false philosophy and that is why Ohio is in such bad shape when it comes to children there.
After his group disappeared, he went on to start claiming to be an expert on election fraud and is the “scientist” that is in one of Mike Lindell’s (My Pillow Guy) crackpot “documentaries” claiming that he has evidence for election fraud using a “6th degree polynomial” that has been repeatedly debunked. He parades Christianity and patriotism as a means to continue fooling his followers. His platforms of choice are now Telegram, Rumble, and other dubious sites.
His specific words about the pandemic and links to rebuttals to his election fraud conspiracy are available online if you are curious.
So what is the take home message if in fact this hypothesis is right concerning hepatitis? It means we aren’t doing a good job at protecting our children, or pretty much a lot of people in American society. The cases of pediatric hepatitis also suggest that there are other chronic conditions that are likely to show up among those with a history of COVID infection in the future. Many have already been emerging.
Here are my recommendations:
- Resume mask mandates in public spaces, particularly in schools, but also in workplaces.
- Educate the public on the need for respirators, not just cloth masks. Even better, get these in the hands of the public using the Defense Production Act and make them freely available to those who might not be able to afford them. Have stockpiles of them available in the appropriate sizes for children in schools as well.
- Improve ventialtion indoors by increasing the number of air changes per hour.
- Add HEPA filtration systems to air handlers and make Corsi-Rosenthal boxes readily available in schools and workplaces to help reduce viral particles in the air since this disease is airborne. In addition, promote their use as a means to keep family members safe if one is currently infected.
- Get the vaccine approved for those under age five.
- Encourage vaccine manufacturers to get variant- and subvariant-specific vaccines in the pipeline when they are emerging, such as omicron BA.4 and BA.5 in South Africa.
- Keep all of these measures in place until the END of the pandemic. The claims that we are in the “endemic phase” are simply false.
If we fail to take these measures, the health, social, and economic consequences will be worse for each that isn’t in place.
Finally, if anyone is interested in doing a multivariate analysis of the data for publication, I would be more than interested in coauthoring that with you.
States with Pediatric Hepatitis Cases and Counts (if available)
Alabama (9) The first report the CDC issued on the mysterious hepatitis focused on a cluster of nine cases spread across different parts of Alabama.

Arkansas (1) Arkansas Department of health is “investigating one potential case, but more investigation is necessary,” a statement to TODAY read.

California (7) The California Department of Public Health told TODAY in a statement on May 5 that it has “received reports of seven young children in California with severe hepatitis since October 2021. We do not know yet if adenovirus played a role in these rare illnesses or if these cases are connected.”

Colorado (4) After asking health providers in late April to start reporting cases of pediatric hepatitis with an unknown cause, the Colorado Department of Health told TODAY in a May 5 statement that it received one reported case that dated back to December 2021. The child was under 10 and tested negative for adenovirus at the time.

Delaware (1) One case is being investigated in Delaware, NBC News reported in late April.

Georgia (handful) The health department in Georgia said it was also investigating a “handful” of cases as of late April, according to NBC News.

Idaho (2) The Idaho Department of Health is currently investigating two cases pediatric acute hepatitis of unknown origin, it told TODAY in a statement.

Illinois (3) The Illinois Department of Health announced in late April that it is investigating “three suspected cases of severe hepatitis in children under ten years of age, potentially linked to a strain of adenovirus. Two of the cases are in suburban Chicago and one is in Western Illinois.”

Louisiana (1) In late April, NBC News reported one case was being investigated in Louisiana.

Michigan (2) Two patients in Michigan meet the CDC’s criteria for being investigated as possibly part of the outbreak, a spokesperson for the Michigan Department of Health and Human Services told TODAY.

Minnesota (3) The Minnesota Department of Health is investigating “several cases” of hepatitis in kids with an unknown cause, local NBC affiliate KARE 11 reported in late April.

New York (handful) New York health officials are investigating a “handful” of cases of hepatitis in kids with an unknown origin, NBC News reported in late April.

North Carolina (2) Two cases of the rare liver inflammation were reported in school-age children in North Carolina, local NBC affiliate WCNC reported in late April.

North Dakota (1) A child in Grand Forks County is recovering at home after being hospitalized with hepatitis with an unknown cause, the North Dakota Health Department announced Thursday.

Ohio (6) Doctors at Cincinnati Children’s Hospital in Ohio told NBC News that they had treated at least six cases in kids between 18 months and 10 years old, all of whom were from Ohio. One child needed a liver transplant.

Pennsylvania (multiple) The Pennsylvania health department is investigating “multiple cases for a possible connection” to the ongoing pediatric hepatitis outbreak of unknown origin but has not confirmed any, according to a statement to TODAY.
South Dakota (1) The South Dakota Department of Health is investigating a case in a child under 10 years old in Brown County, it announced Wednesday.

Texas (cases) University of Texas Health San Antonio has “seen cases of a mysterious and serious liver disease in otherwise healthy children” in South Texas, according to a statement.
The Texas Department of State Health Services told TODAY in a May 6 statement that the state has no confirmed cases of pediatric hepatitis associated with adenovirus 41. “We are aware that some local health departments are investigating cases of pediatric hepatitis to determine if they are associated with adenovirus type 41,” it said, adding that the investigations are ongoing.

Wisconsin (4) As of late April, the Wisconsin Department of Health is investigating at least four cases of unusual hepatitis in children, including one death and one liver transplant.
States with No Confirmed Cases – This may mean that cases are under investigation.
Florida — no confirmed cases

South Carolina — no confirmed cases

States with No Reported Cases (others not listed had not responded)
Maine — not investigating any cases

Mississippi — not investigating any cases

Montana — not investigating any cases

Nevada — no reported cases

Oklahoma — not investigating any cases

Rhode Island — no reported cases

South Carolina — no confirmed cases

Vermont — no reported cases

Virginia — no confirmed cases

Wyoming — not investigating any cases